C4 for Doctors For interested physicians and patients. INTRODUCTION A person can become ill as a result of numerous abnormalities and injuries. Likewise, the motion segments of the spine can be dysfunctional and cause pain or functional disturbances. Although the neuro-articular pathology of the motion segment is highly complex, the clinical experience (with approximately 25,000 patients) has demonstrated that chiropractic treatment can be very effective in lifting a number of well-defined dysfunctions.In this presentation we first discuss the anatomical and physiological properties of the C3/C4 and C4/C5 motion segments. We then proceed with a description of the causes and consequences of dysfunctions (subluxations) and provide a short explanation on how to form a diagnosis. Finally, we conclude with a look at possible treatment modalities and suggestions for future research in chiropraxy.
ANATOMY OF MOVEMENT SEGMENTS
A motion segment consists of two vertebrae that are connected to one another through an intervertebral disc and guided by facets. We will briefly discuss the various components of the motion segment by means of the following images: Fig. 1 & 2 - The top two vertebrae exhibit ante-flexion, causing the intervertebral to be pressed backward. Between the second (green) and third cervical vertebra (blue) we can find the intervertebral disc in its correct location. Between the two blue vertebrae, the motoric segment is suggested. When stretching (lordosis) the vertebrae, the facets end up leaning into each other (the blue one sinks in the purple one). The two lower vertebrae show the location of an in-and outgoing nerve that is surrounded by the dura sheath and which lies in the intervertebrate canal. The intervertebral disc consists of three parts:
- The nucleus pulposus consists of collagen, proteoglycans and various substances that attract water, enabling the nucleus pulposus to function as a shock absorber.
- The annulus fibrosus is layered concentrically around the nucleus pulposus and contains nociceptors. Each of the 15 to 25 concentric annular layers consist of a network of collagen fibers crossing obliquely at alternating angles between adjacent layers [1] and are embedded in the endplates.
- The cartilage endplates consist of two thin, porous, avascular barriers between the vertebral body and intervertebral disc. They regulate the transport of nutrients in and out of the intervertebral disc [3].
The spine owes its flexibility to the presence of so-called facets: moveable joints that connect the vertebrae to one another. They have capsules, richly innervated, that are quite lax and enable a sliding movement. The facets are connected to the vertebral body (lamina and the pedicle). (2)
On the posterior side-edges of the top surfaces of C4 and C5 we can find the uncinate processes also known as joints of Luschka: hook-shaped parts that articulate with C3 and C4. On both sides of the vertebral bodies, at the level of the in-and outgoing nerves, we can find the so-called transverse apophysis. Several muscles, including the rotator muscles, attach themselves to the laminae and Istmis. The vertebral artery passes through small channels in the apophysis and is surrounded by sympathetic nerve fibers. The latter are in contact with the distant sympathetic stellate ganglion. Fig 4 & 5 - Viewed from in the spinal canal. A longitudinal ligament can be seen on the rear wall of the vertebral bodies and spread across the sheaths of the disc. This ligament starts from the cranium and reaches far into the thoracic part of the spine. We can distinguish several ligaments that bridge - and attach to - the various vertebrae, namely the anterior and posterior longitudinal (fig 4 & 5) ligaments, the yellow ligaments, the interspinous and supraspinous ligaments. These ligaments strengthen the joint but do not have enough traction to guarantee stability. As such, additional muscle power will be needed. Some of these ligaments run from endplate to endplate, through the nucleus pulposus [1]. The spinal cord is located in the spinal canal. At the level of C4/C5, the sagittal diameter of the spinal canal measures a minimum of 12 mm and the lateral diameter 22-mm [13]. It contains lateral canals in which the low-lying, outgoing, thin motor nerves and the higher up sensory nerves (nervus sinu) are situated. The spinal cord contains the Rolando's substantia gelatinosa of the trigeminal sensory nerve of the face (forehead, cheeks and throat) as well as the motor cells of the neck muscles: the scaleni, arms, biceps, triceps, forearms and hands, shoulders, deltoid and diaphragm. The spinal path of the trigeminal extends at least up to segment C3, possibly even C4 [31]. (Convergence of the trigeminal afferents and cervical afferents on the trigeminocervical complex). 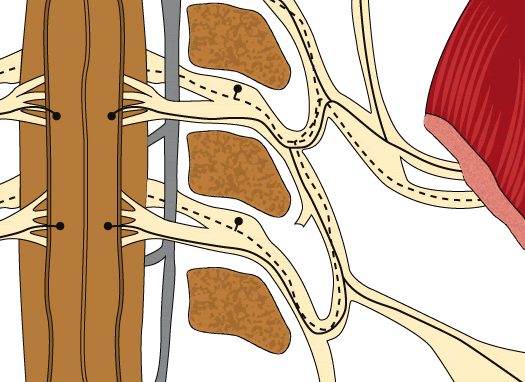 Fig 6 - This drawing suggests the course of the motor and sensory nerves from the spinal cord to a shoulder muscle at the level of C3 / C4 / C5. The spinal cord contains the front part responsible for the movements of the body and the rear part responsible for feel and sense of touch. Fig 6 - This drawing suggests the course of the motor and sensory nerves from the spinal cord to a shoulder muscle at the level of C3 / C4 / C5. The spinal cord contains the front part responsible for the movements of the body and the rear part responsible for feel and sense of touch. Innervation of the intervertebral disc, dura mater and posterior longitudinal ligament.
The dorsal sensory ganglion, usually located in the central upper part of the intervertebral foramen, innervates the dorsal part of the intervertebral disc through the sympathetic stems and sinuvertebral nerves [13]. The sensory fibers are distributed segmentally over the dural sleeves. Fibers in the posterior longitudinal ligament extend beyond the segmental boundaries. Sympathetic fibers are distributed across the arterial walls and also across regions that are independent of the arteries, the cervical dura mater and the posterior longitudinal ligament. Some sympathetic fibers run alongside sensory fibers. Clinical symptoms can be attributed to this characteristic innervation of the cervical spine [11].  Fig 7 - The sympathetic nerve fibers of the sympathetic (stellate ganglion) to the vertebral artery (drawn in yellow). Fig 7 - The sympathetic nerve fibers of the sympathetic (stellate ganglion) to the vertebral artery (drawn in yellow).
The roots of the nerves are closely tied to the pedicles and are not static. When the spine and the limbs move, the spinal nerves and nerve roots adjust to the change of the spinal position. They do so by stretching, loosening or shifting into the vertebral foramen. 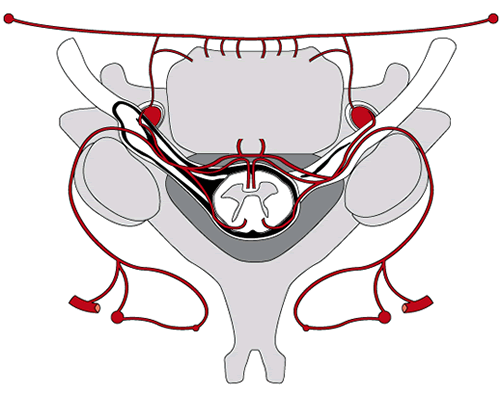
Fig. 8 - The blood vessels and capillaries (drawn in red)
penetrate into the vertebral bodies as well as anterior and posterior of the spinal cord.The nerve fibers also have a rich vascular supply: the peripheral nerves have a well-developed microvascular network, while the blood supply of the ganglia of the nerve roots and spinal nerves runs through segmental arteries and medullary veins. Arteries enter through the poles of the ganglia, where they penetrate the dural sheath. The veins exit through the periganglionic plexus. Inside the ganglion we can find arterioles, capillaries and venules. Almost every nerve cell in the ganglia seems surrounded by a capillary loop. When the nerve is stretched, venular stasis is induced. From the joint capsules three important types of mechanoreceptor fibers stretcth to the spinal cord [2]. They can span several motion segments and provide proprioceptive information about pain, position and tension,(capsular and ligamentous fixation) and also regulate the stability and power of the small muscles. PHYSIOLOGY OF THE MOTION SEGMENTS (1) Movement:
The movement between two vertebrae occurs along 3 axes: - the coronofrontal shaft is located at the rear of the intervertebral disc. When bending the neck, the diameter of the inter-vertebral canal grows larger (+10%) and the spinal cord is extended. Through extending, the diameter becomes 13% smaller. .
- the sagittal axis for lateral flexion movements runs through the nucleus pulposus
- the vertical axis for torsional movement (in the neck) lies in the vicinity of the posterior longitudinal ligament and is very dependent on the shape and direction of the upper facets.
(2) Nutrition:
The nucleus cells of an adult intervertebral disc only produce ATP (energy) through the process of glycolysis. They consume glucose and lactic acid at a high rate and do not seem to need much oxygen. The main part of the intervertebral disc - with the exception of the annulus - is supplied with nutrients by the vertebral blood vessels and capillaries (24-15) These blood vessels penetrate the subchrondral plate and end in the cover plate. Loss of nutrients seems to occur mainly through calcification and/or sclerosis of the cover plate. This increases with age and degree of degeneration.
For its survival the axon of a nerve depends on the physiological connection to the cell body of the neuron. Within the axons of the peripheral nerves, there is a continuous transport of substances (e.g. proteins and organelles) to and from the cell body and the ends of the axons. Various neuropathies are linked to failures in this transport system, for example, toxic, ischemic or traumatic disorders of the peripheral nerves [4].
(3) Hydration:
The intervertebral disc absorbs water, especially at night when lying down. When standing up, water is squeezed out of the intervertebral discs. The intervertebral disc undergoes daily changes in the intradiscal pressure, depending on the different day and night activities. Upright positions and load-bearing activities cause high load pressure; lying positions cause low load pressure. Under high load, the intervertebral disc deforms and the hydrostatic pressure within the intervertebral disc increases, slowly squeezing water out of the disc. This causes an increase in the concentration of proteoglycans. In supine position, water is again reabsorbed. Every 24 hours, about 25% of the water content of the intervertebral disc is expelled and reabsorbed. The loss of water after 1 hour of running corresponds to the total loss of water in a normal upright daytime activity [3].
SUBLUXATION: CAUSES & CONSEQUENCES
Subluxations: dysfunctions in the mobility and neurophysiology of motion segments, may occur in case of:
- Direct mechanical pressure on the spinal nerves and blood vessels
- Spasms in the muscles that surround the joints
- Fibrosis of the facets and/or ligaments
In conventional medicine, the word subluxation is now also used when a radiologically observable, albeit minimal, displacement of a disc has occurred. We briefly discuss the causes and consequences of each of these three elements. 1) A Direct mechanical pressure on the spinal nerves
Compression of a spinal nerve can lead to a deformation of the nerve fibers, especially at the edges of the compressed segment. When nerve injuries occur, one can often observe an intra-neural edema as the intra-neural microvessels respond to compression trauma by increasing their permeability. The nerve roots, however, are protected because they are surrounded by a cerebrospinal fluid which, together with the dura and the arachnoid membrane which forms a buffer against compression. Pressure on the nerve can block nerve conduction, thereby causing a disruption of both the transmission of impulses and the transfer of key substances from the cell bodies to the periphery of the axon. Prolonged blockage of the nerve leads to Walleriaanse degeneration. The closer to the cell body the more severe the degeneration [4, 5] and neuropathy. The functional changes that can be observed during compression of a nerve include loss of nerve function manifested as muscle weakness, lack of sense perception or a state of hyper-excitability of the nervous tissue. This gives rise to pain, paresthesia (dysfunction of the tactile sensation), motor dysfunctions, dysfunctions of numerous nerves and reflexes (deltoid, triceps, biceps tendon) and possibly muscle fasciculation (6). 1) B If the pressure is caused by a broad, central, disc hernia - an injured nucleus pulposus would produce cytokines and other neurotoxic products - then pressure on the spine would be anteroposterior. In this case, the nerve tracks that are first affected are the long posterior nerves in the spinal cord. These Goll- and Burdach-tracks can then show symptoms like paresthesia on the soles of the feet, pallidal (loss of sense of vibration), Babinski sign, sign of Hofmann, sign of Trömner and anuria. The sign of Trömner is a well-documented neurological sign of pyramidal response [12]. It is a flexion of the thumb and index finger in response to the "tapping / flicking" of the volar (palmar) surface of the distal phalanx of the middle finger that is held partly bent between the finger and thumb of the researcher. The Trömner and Hofmann signs are used as a clinical neurological test for lesions of the upper motor neurons above C5/C6. Also stenosis of the spinal canal, due to hypertrophic yellow ligaments and arthrotic spurs, can interfere with the normal circulation of the cerebrospinal fluid and so induce headaches and lethargy. 1) C Studies have shown that the blood flow in the nerve root is reduced when the nerve is compressed in vivo [6]. Degeneration at the level of the compression is accompanied by an expansion of the degeneration in the primary sensory neurons in the dorsal root ganglion (7). (With degeneration the number of neurons with central chromatolysis increased and in the cytoplasma there was dissolution of the Nissl bodies and the mitochondria showed vacuolisation) (7)Acute stretching of peripheral nerves inhibits retrograde axonal transport. This is mainly caused by a disturbance of the circulation [22]. Intra-radicular edema is caused by an alteration of the blood-nerve barrier and is the main cause of dysfunction of nerve root under chronic compression [21].
2) Spasm in the muscles that surround the joints

Fig. 9 - From the front part of the spinal cord, nerve fibers leave towards the muscles (alpha motor neurons) and thinner fibers (gamma motor neurons) leave towards the spindles in the muscle mass. Conversely, sensory nerves (proprioceptive fibers 1a) leave from the muscles (Golgi 1B fibers) and from the spindles, returning to the back part of the spinal cord. These inform the spinal cord on the stress state of the muscles and the small spindles. The balance between these two systems enables a normal contraction or relaxation of the muscles. From the joint caps (missing here), sensory nerves ( mechanoreceptors) leave and may be the triggering factor of abnormal muscle tension.
When the short muscles surrounding the joints go into spasm, it causes an increased pressure on the motion segment. This may cause a vicious cycle of muscle spasm - nerve irritation - muscle spasm [19] and not only leads to pressure on the nerve but also to pressure on the facets.
3) Fibrosis of the joint capsules and / or ligaments
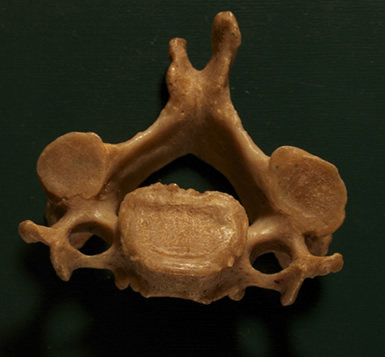 Fig. 10 - Osteophytes can be observed at the posterior side of the motion segment. Fig. 10 - Osteophytes can be observed at the posterior side of the motion segment.
An abnormal movement can cause small cracks in the capsules of the facets which later become inflamed. When such an inflammation heals, some scar tissue of type III collagen or osteophytes may be formed. This tissue can inhibit or interfere with the normal motion of the joint [16-18-24).
SUBLUXATION: DIAGNOSIS
To proceed to a treatment, the chiropractor will first try to exclude a host of other pathologies (tumors, bone diseases, psychiatric pathologies, etc.) by means of a standard clinical examination. Pain - in and of itself - is not a valid criterion for medical treatment. The so-called "silent killers" such as lung- and pancreatic cancer can be painless while very painful conditions exist that have no known causes or where the cause of the pain is psychic.
Since an MRI is not invasive and is used daily in the clinical setting, it seems a very suitable method to observe stenosis of the intervebral foramina, the spinal canal diameters and changes in the intervertebral disc. In NMR tests, T1 rho is correlated with water content and inversely correlated with age and degeneration of the intervertebral disc. The mechanical function and water content of the intervertebral disc depends on the collagen and proteoglycans. Water content is related to the osmotic pressure caused by the fixed negative charge of the proteoglycans while the unique structure of the collagen fibril offers resistance to swelling. But an MRI is usually taken while the patient is lying down and the intervertebral discs are relatively unloaded. MRIs taken in standing position would be more useful [3]. Future developments in MRI will be able to provide more accurate information (15-17).
 Fig.11 - Three discal hernias of various sizes causing a displacement of the spinal cord. The patient died of "lateral amyotrophic sclerosis": a condition of the spinal medulla. Fig.11 - Three discal hernias of various sizes causing a displacement of the spinal cord. The patient died of "lateral amyotrophic sclerosis": a condition of the spinal medulla.The classic symptoms of general pressure on the cervical spinal cord (usually symptoms of exclusion for the chiropractor) are: paresis of the upper limbs (atrophy of the small muscles of the hands) and lower limbs, gait disturbance (tetraparesis), pathologically increased muscle-tendon reflexes, sensibilities abnormalities and sphincter disorders. When these signs of myelopathie occur and persist, it is a medical error not to carry out a neurosurgical procedure. This is for medullary complaints.(8) In addition to an MRI scan, Doppler studies may be of interest to the chiropractor as they can detect decreased blood flow in the blood vessels. Mechanical pressure on the blood vessels (arteria vertebralis) can indeed be caused by distorted facets, calcified annuli, thickening of the ligaments or bad alignment of the vertebrae (very rarely) resulting in dizziness. Also usefull in the examination is bone scintigraphy aiming at clarifying articular or bone or other pathologies.
Movement palpation
The manual examination with the fingertips of the mobility of the intervertebral motor segments is central and fundamental for the Chiropractor.
To detect a subluxation, one must first estimate the mobility of the motion segment. This is done by comparison with the adjacent segments. Each individual segment has its own degree of "stiffness". The comparison with neighboring segments is therefore usually very suitable as a yardstick.  Fig.12 - Narrowing of the intervertebral canals due to osteophytes. Fig.12 - Narrowing of the intervertebral canals due to osteophytes.
(1) Direct mechanical pressure on the spinal nerves
Following a general neurological examination and on the basis of tests that include a nerve stretching, one can usually confirm exactly where the nerve is compressed. Eg: Ulnar nerve stretch: by abduction of the shoulder at 100° with the elbow flexed to 130°. Radial nerve stretch: by abduction of the shoulder at 110° with the elbow fully extended with a pronated forearm. The cervical nerve root stress test : shoulder is abducted at 90° with the elbow slightly flexed and a postero-anterior pressure is applied on the humeral head with retroversion of the arm to 30° (35) The cervical test may also be enhanced by lifting the head in ante-flexion (Lhermitte's sign: Whereby the spinalcord and the nerves are being streched over their entire lenght and by canaal stenosis produce electic discharges in the extremities. Bending sideways, one can also notice a (local) iso-lateral mechanical restriction. This inhibition can be caused by a hernia, an edema, a varicose venule or osteophyte. (2) Spasm in a muscle surrounding the articulation produces a springy restriction of movement in a specific direction. Fig. 13 - We can see that the surfaces of the joints are elongated
due to asymmetrical postures or reflectory muscle spasms
(3) Fibrosis of the joint capsule and/or ligaments
One can detect such fixations (restrictions) by means of a precise palpatory examination of the mobility of the vertebral motion segment above and below C4. This inhibition does not feel springy - as would be the case with a muscle contraction - but stiff.
When bending forward (ante-flexion) one may also discover a shrunken interspinosum and supraspinous ligament (posterior ligamentary complex). This deviation is most common in lordotic women and causes a chronic compression of the small joints.
SUBLUXATION: TREATMENT
In the past 50 years, chiropraxy has been intenselly scientifically substantiated this next to clinical experience and taking into account the numerous placebo effects.
Experience shows that a chiropractic treatment - by stretching the joint capsules, ligaments and muscles (within the physiological norms) - may have an impact on (the collagen fibers, proteoglycans and the connective tissue of) a motion segment. Such a treatment can as such lift the subluxations.
(1)Direct mechanical pressure on the spinal nerves
The surgical and chiropractic treatment of a nerve disorder caused by direct mechanical pressure aims to also lift the pressure on the nerve. Chiropractically this can usually be accomplished through a short, quick, gentle swirling motion on the appropriate vertebra.
Upon rotation of the vertebrae, in comparison with the adjacent vertebrae, the torque of a cephalic vertebra to a lower caudal vertebra can feel restricted . In this case, the joint capsule on the inhibited side can be loosened through a rapid short torsion. The contralateral joints serve as a fulcrum. This process of loosening is usually accompanied by the famous "crack" sound (under pressure). Interruption of the tension between two articular surfaces will likely also cause a reduction in the proprioceptive articular irritation and consequently muscle spasm and nerve compression .
(2) Spasms in the surrounding muscles
A fast, short, stretching movement with high torque, low amplitude and low force can ensure that the small muscles surrounding the joints do not have the time to counteract the stretch effect. This causes them to relax and thus the motion segment to be relieved [15, 16]
(3)Fibrosis of the joint capsule and/or ligaments
In the case of older joint capsules it is often sufficient to stretch these very quickly. Younger fibrosed joint capsules are often protected by muscle spasms. In the majority of cases a brief, light jerking movement in the right direction is often sufficient to liberate the motion segment and the mechano-receptors.
When stretching the spine (backward bending), the Chiropractor may feel an inhibition of movement between two adjacent vertebrae. From the feel of the inhibition he can deduce whether it is located in or near the anterior longitudinal ligament. Normal mobility can be restored by means of a short push in the proper direction. It is almost like loosening a velcro ligamentous structure. The neurological and subjective symptoms are also often resolved in this manner.
In the case of a shrunken interspinosum (posterior ligamentary complex) ligament, a correct, locally-targeted traction can loosen the fixation. Normalization of the mobility between two vertebrae also leads to normalization of discal protrusions and extrusions, thanks to the stretching of the posterior longitudinal ligament. Experience shows that after mobilization of the vertebrae, the nerves are probably minimally shifted such that the symptoms disappear, even if the radiological images do not indicate such.
The question of whether a fixation of two vertebrae may be the cause of hyper mobility and degeneration of the surrounding joint, has been repeatedly posed in scientific articles. It appears conversely, that the release of a capsular fixation on one level (e.g. C5/C6) can improve the (hyper) mobility of an adjacent vertebra and relieve the neurological signs and symptoms at C3/C4, both in terms of feeling and mobility. It is clear that further research is needed to better understand the complexity of subluxations. 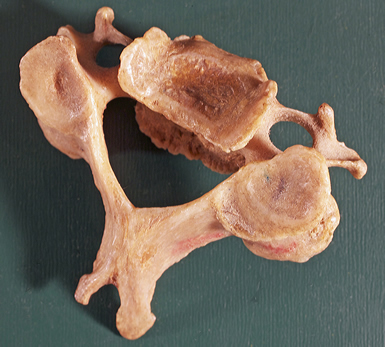
Fig. 14 - We can see that the surfaces of the joint are extended (elongated)
due to a tenuous asymmetric posture. The aforementioned diagnostic tests can objectively confirm the rapid improvement of the patient, supplemented with subjective information provided by the patient himself. As for long-term abnormally held postures, it is possible that the joint surfaces become deformed. Since the entire mechanical chain needs to find a new relaxed physiological balance, repetition of treatment of the primary subluxations is recommended. More recent problems usually require only a small number of interventions this when carried out by an experienced practitioner having daily experience. In unqualified hands, manipulations of the joints can lead to deterioration and permanent damage. Usually, with few exceptions [29], it is claimed that a surgical procedure is applied after the failure of "conservative" therapies. Is this the case and have all neuro-chiropractic opportunities been used? Today, the highly acclaimed neuro-surgical procedures have high success rates for discoradicular conflicts, but when neurosurgical interventions are applied to complaints of the neck, they still only achieve 60% success. This is important to note, considering their cost to society is approximately € 10,000 where a successful chiropractic treatment would cost the patient only € 150 to 200 out of pocket.
CONCLUSION
Clinical experience shows that despite the complexity of the neuro-articular physiology and pathology of the motion segments C3/C4/C5, neuro-chiropractic treatment can be very effective for lifting well-defined dysfunctions such as subluxations. During chiropractic treatment (high velocity, high torsion, low amplitude, low force adjustment) the ligaments are slightly stretched causing a positive effect on the disc protrusions, thereby broadening the intervertebral canals, lifting the edema and varicosities. This also improves the rehydration of the discs by means of the slight but prolongated traction. This risk-free efficiency is useful for both the patient and the physician who refers the patient to a chiropractor. From an ethical viewpoint, it also serves the society financially.
Sincere thanks and appreciation for their collaboration:
Prof. Myriam van Moffaert (Psychiatrist)
Sarah Verschueren: (PhD Biomedical Physics, Msc Cell Engineering)
Monique Sluyts (Webdesign)
Roger de Paepe (Journalist)
Dr. Ates Recai (Neurosurgeon)
Prof. Marc de la ruelle (Germanic Languages Expert)
Dr. Bernard Koentges (Vascular Surgeon)
Emmanuel Balan (Infographic Artist)
Prof. Cécile Krings (Romaniste)
BIBLIOGRAPHY (1) Wade, R.K. et al. (2011) A fresh look at the nucleus-endplate region: new evidence for significant structural integration. Euro Spine Journal. 20(8), 1225-1232. (2) Windsor, R.E. et al. (2012) Cervical facet syndrome. Medscape. Jan 13. (3) Chan, S.C. et al. (2011) The effects of dynamic loading on the intervertebral disc. Euro Spine Journal. 20(11), 1796-1812. (4) Rydevik, B. et al. (1980) Blockage of axonal transport induced by acute graded compression of the rabbit vagus nerve. Journal of Neurology, Neurosurgery and Psychiatry. 43, 690-698. (5) Rydevik, B. et al. (1983) Pathoanatomy and pathophysiology of nerve root compression. Department of orthopaedic Surgery, Sahlgren Hospital Göteburg. March 16. (6) Shigeru, K. et al. (2003) Changes in nerve root motion and intraradicular blood flow during an intraoperative straight-leg-raising test. Spine. 28(13), 1427-1434. (7) Kobayashi, et al. (2004) Morphological and immunohistochemical changes of dorsalroot ganglion after nerve root compression. Journal of Orthopaedic Research. 22(1), 180-188. (8) Dvorak, J. et al. (2003) Cervical myelopathy: clinical and neurophysiological evaluation
European Spine Journal. 12(2), 181-187. (9) Zhang, Y.H. et al. (2011) Cyclic strech-induced apoptosis in rat anulus fibrosis. European Spine Journal. 20(8), 1233. (10) Aebi, M. (2010) Surgical treatment of upper, middle and lower cervical injuries…
European Spine Journal. 19(1), S33-S34. (11) Yamada, H. et al. (2001) Comparison of sensory and sympathetic innervation of the dura mater and posterior longitudinal ligament in the cervical spine after removal of the stellate ganglion. Journal Comp Neurology. 434(1), 86-100. (12) Chang, C.W. et al. (2011) Quantification of the Trömner sign: a sensitive marker for cervical spondylotic myelopathy. European Spine Journal. 20(6), 923-924. (13) Morishita, Y. et al. (2009) The relationship between the cervical spinal canal diameter and pathological changes in the cervical spine. Euro Spine Journal. 6, 877-883. (14) Takahashi, K. et al. (2008) Resolving discogenic pain. The Intervertebral Disc European Spine Journal. 17(4), S428-S431. (15) Kandel, R. et al. (2008) Tissue engeneering and the intervertebral disc. The Intervertebral Disc European Spine Journal. 17(4), S485-S487. (16) Kallakuri, S. et al. (2008) Tensile streching of cervical facet joint capsule and related axonal changes. European Spine Journal. 17(4), 556-563. (17) Mwale, F. et al. (2008) Quantitative MRI as a diagnostic tool of intervertebral disc matrix composition and integrity. The Intervertebral Disc European Spine Journal. 17(4), S432-S440.
(18) Maffuli, N. et al. (2000) Tenocytes from ruptured and tendinopathic Achilles tendons produce greater quantities of type III collagen than tenocytes from normal achilles tendons. American Journal of Sport Medicine. 28(4), 499-505.
(19) Wolff, H.D. (1983) Neurophysiologische Aspekte der manuellen Medizin (2nd Ed.) p19-28. Springer-Verlag. (20) Tanoue, M. et al. (1996) Acute streching of periferal nerves inhibits retrograde axonal transport. Journal of the British Society of Surgery of the Hand. 21(3), 358-363. (21) Hidezo, Y. et al. (1995) Chronic Nerve Root compression: pathophysiologic Mechanism of Nerve Root Dysfunction. Spine Journal. 1995/ 02001 (22) Bakhatdze, M.A. et al. (2012) Cerebral perfusion in patients with chronic neck (…) pain.
Journal of Manipulative and Physiological Therapeutics. 2012;35(2), 76-85 (23) Haavik, H. et al. (2010) The effects of spinal manipulation on central integration of dual somatosensory input observed after motor training. Journal of Manipulative and Physiological Therapeutics. Page: 261. (24) Stefanakis, M. et al. (2012) Annulus fisures encourage blood vessel and nerve ingrowth into degenerated intervertebral discs. Spine Journal Supplement. 2012, S232. (27) Walter Herzog, Conrad Tang. August 2012. Internal carotid artery strains during high-speed low amplitude spinal manipulations of the neck. Journal of manipulative and physiological therapeutics. (28) Yanlin, T. et al. (2012) Kinetic MRI analysis of lumbar segmental mobility Pfirrmann grading. Euro Spine Journal 21:2673-2679 (29) van Midddelkoop, M. et al. (2013) Surgery versus conservative care for neck pain: a systematic review. Euro Spine Journal 22:87-95 (30) Bartsh, T. et al. (2003) The trigeminocervical complex and migraine. Current pain and headaches report 2003 volume 7, issue 5, pp 371-376 ( Institute of neurology, Queen Square Londen UK) (31) Bogduk, N. et al. (2001) Cervicogenic headache: anatomic basis and pathophysiologic mechanisms. Current pain and headaches reports 2001 volume 5, issue 4, pp 382-386 (Newcastle Bone and joint Institute, Australia) (32) Vital JM, et al (1983) Anatomy of the lumbar radicula canal. anat.clin 1983:5 141-145. (33) Panjali MM et al (1983) Kinematics of lumbar intervertebral foramen.
Spine 1983:8-348-357. (34) Vital JM et al (2003) Anatomy of the normal congenitally narrow & degeneratively narrow lumbar canal. Cahiers d'enseignement de la Socat:2003:83:1-18. (35) Farshad M, Min K (2013) Abduction extension cervical nerve root stress test. Eur Spine J (2013) : 22:1522-1525
© copyright Back to top
| 


